By Isanella Patoir
March 11, 2021, marks exactly one year since Guyana recorded its first COVID-19 case and death. To date, 205 persons have died of the 8,928 who have tested positive while a total of 8, 211 have recovered.
With a rush of vaccines into the country now, could this be the beginning of the end of the pandemic here?
For the many who have lost loved ones, even the grieving process has been as strange and frightening as the pandemic – no large funerals meant the absence of the usual comfort of family and friends. Celebrations – birthdays, graduations and marriages – were all reduced to small gatherings.
Fifty-two-year-old Ratna Baboolall from Good Hope, East Coast Demerara was the first confirmed case and death in Guyana. She died on March 11, 2020, days after she arrived in the country from the United States with her husband and children. The Baboolall family is also recorded as the first group of persons to test positive for the virus here.
The majority of the deaths from the virus were recorded in Region Four, (Demerara-Mahaica) – the largest populated region in the country- and according to health officials, everyone who died suffered from underlying conditions or what can be referred to as comorbidities.
A retired nurse of the Georgetown Public Hospital lost his battle to COVID-19 on October 05, 2020. The nurse, Mark King, was 55-years-old. He was last stationed in the Accident and Emergency Unit and doctors said he was one of the best nurses to work with. King retired in July 2020.

King had underlying conditions and was admitted to the COVID Intensive Care Unit on September 25, 2020. His father, Kenneth King, during a recent interview with the News Room, said he was not aware of the extent of his son’s illness.
“He complained of being sick at times and went to the doctor, and eventually, he ended up at the hospital. His sickness was, I wouldn’t say long, but a few weeks and I was surprised and taken back at his death,” the father said.
King lived with his father in Albouystown, Georgetown.

A six-day-old baby with a heart condition and an 11-year-old with Leukemia were both recorded as the country’s child deaths from the virus. The oldest person to survive COVID-19 in Guyana is Zorie De Mattos. De Mattos, who is a resident of the Palms Elderly Care Facility, is 106-years-old.
Within a few weeks of the pandemic, many lost their jobs and were laid off and even now businesses continue to suffer as a result of the pandemic. But despite the pandemic and the protracted general and regional elections, Guyana’s economy grew by 43.5 per cent in 2020, giving hope that the nation can bounce back from the overarching ramifications of the dreaded disease.

The growth was driven by the burgeoning oil and gas sector. The year 2020 was the first full year of Guyana’s oil production and it is for this reason that such a massive growth was recorded.
In recent months, the National COVID-19 Task Force granted approval for non-essential businesses such as resorts, bars and restaurants to reopen with strict measures and limited capacity.
The government further extended the National COVID-19 measures for the month of March, which means that restrictions against social activities remain in place and the 10:30 p.m. to 4 a.m. curfew is still in effect. The restriction on private parties, wedding receptions, wakes and the usage of hotel pools also remain in effect.
RESPONSE TO THE PANDEMIC
Meanwhile, the Doctor-in-Charge at the Infectious Diseases Hospital (COVID-19 Hospital) located at Liliendaal, East Coast Demerara, Dr Tracey Bovell, said the growth in knowledge and capacity in the health sector has been tremendous.
“I have seen the health sector grow, not in the number of persons as in the number of staffing increasing, but I have seen the health sector grow in mentality and capability,” Dr Bovell explained.
Dr Bovell has been serving the health sector for the past 13 years and prior to the pandemic, she was the Emergency Medicine Specialist Trauma Coordinator at the Accident and Emergency Department of the Georgetown Public Hospital.
Even before the first set of confirmed cases in the country, Dr Bovell said preparations had started months earlier in anticipation of the virus. She said while the health sector was preparing for mass casualty, the health workers had their fingers crossed that the virus would not enter Guyana.

“…then March 2020 happened and we had our first patient and with our first diagnosed patient, we had our first death in Guyana and that really brought us into the reality that COVID-19 is coming and even with our first case we still did not think that the pandemic would last so long,” Dr Bovell explained.
She highlighted that it was scary at the time, in terms of not knowing what to expect with patients, how to treat them and their complications with the virus. But with experience, exposure, evidence-based medicine and scientific studies, the health workers are now better positioned in their response to the pandemic.
All of this was further complemented with the completion of the COVID-19 Hospital in July 2020. Before the completion of the hospital, COVID infected patients were being treated at the Georgetown Public Hospital.
“Initially, when we started thinking of COVID in January [2020] at the Georgetown Public Hospital, there was no facility in mind and we started to create spaces to cater for COVID patients,” Dr Bovell explained.
Now, the COVID Hospital is far more equipped to deal with a wide range of COVID-19 patients – from maternity to pediatric and persons with mild to severe symptoms of the virus. A clinical group has also developed specific guidelines on how to treat COVID patients. These protocols and guidelines have since been standardised and adopted in hospitals across the country.
HOPE
With the development of a number of vaccines, there is now hope that the end of the pandemic is near. But Guyana still has a long way to go in order to achieve herd immunity and be COVID-19 free. And with every passing day, the Ministry of Health is reporting new cases. Dr Bovell is among the first set of doctors who received the Oxford-AstraZeneca COVID-19 vaccine.
“We have the vaccine and I am hoping things will start looking up. I am hoping that everyone can get vaccinated and ensure that they have protection and we can continue getting better from here on,” Dr Bovell said.
The largest batch of COVID-19 vaccines arrived at the Cheddi Jagan International Airport (CJIA) on March 07, 2021; 80,000 doses of the Oxford-AstraZeneca vaccines were donated by the Government of India.
The vaccines from India came days after 20,000 of the Sinopharm vaccines donated by China arrived here. Before the end of the month, Guyana will also receive thousands of vaccines through the COVAX facility and the CARICOM/ African Union agreement.
The country began its COVID immunisation on February 11, 2021, with a donation of 3,000 doses of the Oxford-AstraZeneca vaccine from Barbados; the authorities later granted emergency use approval of the Russian Sputnik COVID-19 vaccine, as well as, China’s Sinopharm vaccine.
Each Guyanese will get to choose whether they want to be vaccinated but the Minister of Health, Dr Frank Anthony, has emphasised that these vaccines are safe and that scientific studies have shown that there are low side effects. It should also be noted that a National Committee was set up to monitor any adverse effects of the vaccines. Persons are still being advised to take the vaccine in order for the country to start its recovery from the pandemic.
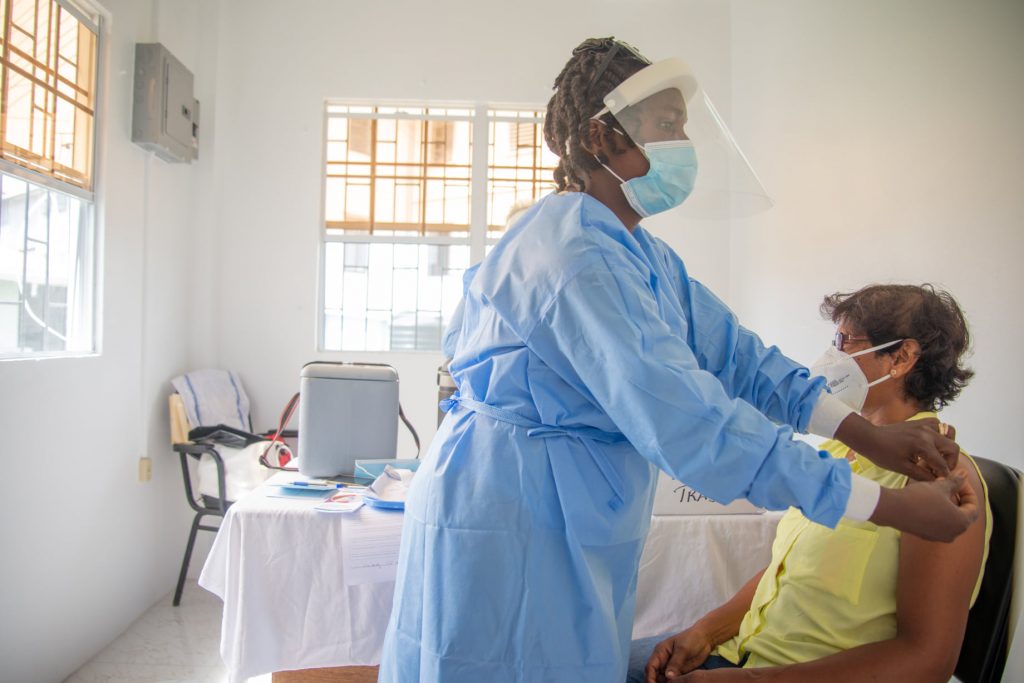
At the moment, frontline health workers, persons 60 years and over are being vaccinated; this will be followed by persons with comorbidities, teachers and members of the joint services.
FRONTLINE WORKERS
Sister Shannon Haynes, who is now a ward manager at the COVID-19 Hospital, was initially stationed at the maternity unit of the Georgetown Public Hospital; she is one of the many health workers who continue to work on the frontlines.
“I was at maternity when COVID started and I was asked by the matron to go up with a group of nurses to open the Ocean View Hospital because of the overcrowding at our maternity department and we did so,” Haynes explained.
Haynes told the News Room that she saw the opportunity to do her part in the fight against the virus. Additionally, she explained that her family and loved ones live in Essequibo and this was more reason to go serve at the COVID Hospital.
“I knew I wasn’t going to put my family at risk in any way because they are there and I am here and I was thinking about the other persons that would have their family and would have to go home to them.”

Meanwhile, many of the indigenous villages in the hinterland regions were placed under lockdowns and were the epicenter for the pandemic. Moruca, located in Region One, Barima-Waini at the beginning of the pandemic was one of the hotspots for COVID in the region.
Dr Derron Moonsammy was stationed at the Kumaka District Hospital in Moruca as the doctor-in-charge at the time. One month after Moruca recorded its first case, Dr Moonsammy tested positive for the virus.
Now one of the 8,000 survivors, he recounted his experiences to the News Room.
“It was very difficult, everybody was moving at a faster pace, we had to find resources and call the right people and then I got sick…I was working with COVID patients, we had 27 patients at the time and I felt unwell,” Dr Moonsammy explained.
Dr Moonsammy said he was working directly with COVID-19 patients and somewhere along the line he took off his mask or maybe forgot to wash his hands. He explained that he first thought it was dengue fever, but a test later confirmed his diagnosis and he was placed in isolation for about a month before returning to work.

The symptoms Dr Moonsammy experienced included shortness of breath, diarrhoea, increased heart rate, high blood pressure, tremors and burning in the nose along with a cough, cold and pain in the back of his eyes. In February this year, he relocated to the Georgetown Public Hospital and no longer works with COVID-19 patients. Nevertheless, he credited the team at the Kumaka Hospital who continue to work tirelessly to ensure the safety of every patient and staff.
IMPROVED TESTING
The National Public Health Reference Laboratory (NPHRL) during the first seven months of the pandemic was the only local certified laboratory to do PCR- COVID-19 tests. With just one certified lab testing for samples for the entire country, the Health Ministry was faced with a huge backlog of samples and this also resulted in results taking longer than usual. Now, two privately owned labs -Eureka Medical and Coastland Diagnostic Centre – are certified to conduct PCR testing.
Additionally, the government has also implemented rapid antigen testing, which is done within 20-30 minutes. GeneXpert machines are also being used to carry out COVID-19 tests; the machines were previously used to test persons for tuberculosis, but have now been recalibrated to test for COVID-19.
The government will soon commence a Serosurveillance study in Guyana to determine the trends with the COVID-19 pandemic here. The study is being done in collaboration with the Pan American Health Organisation (PAHO) and experts from Harvard University. With new and highly transmissible variants of the virus discovered in the United Kingdom, neighbouring Brazil and South Africa, Guyana remains on high alert.

A year later and schools across the country remain closed with only face to face learning for high school students writing CSEC and Cape Exams.
Children continue to be taught via online classes, but in a country with limited access to the internet, this remains a challenge for many parents. There is some hope that schools will re-open after the Easter Holidays as long as a majority of the population is vaccinated against the virus.
From all indications, the Coronavirus will be with us for a long time and the onus is not only on the government to ensure we are safe, but for us to also practice and adhere to all the safety guidelines in order to curb the spread.
Wash your hands frequently, wear your mask and keep your distance. Protect yourself so that you can protect others.






